7 Signs Your OWCP Injury Claim Needs Medical Support

You’re sitting in your doctor’s office, holding a stack of paperwork that might as well be written in hieroglyphics. Your shoulder’s been killing you since that incident at work three months ago – you know, the one where you had to lift that ridiculously heavy box because the forklift was down *again*. The workers’ comp people keep asking for more documentation, more proof, more… everything. And honestly? You’re starting to wonder if they think you’re making the whole thing up.
Sound familiar?
Here’s the thing about OWCP (Office of Workers’ Compensation Programs) claims that nobody tells you upfront: they’re not just about proving you got hurt. They’re about proving you got hurt *enough* to warrant ongoing support. It’s like being asked to defend your pain to a jury of people who’ve never experienced it themselves.
I’ve seen too many folks – hardworking people who’ve given their all to their jobs – get stuck in this bureaucratic maze. They file their initial claim, maybe get some basic treatment approved, and then… crickets. Or worse, they get a letter saying their claim is being “reviewed” or that additional medical evidence is needed. Translation? Your word isn’t enough anymore.
The reality is, your body doesn’t heal on the government’s timeline. That back injury from lifting packages all day doesn’t magically disappear because it’s been six months since you first reported it. Your carpal tunnel doesn’t suddenly get better just because you’ve been doing physical therapy for a few weeks. Sometimes – actually, pretty often – workplace injuries get complicated. They develop into chronic conditions, they affect other parts of your body, or they just plain refuse to heal the way the textbooks say they should.
And that’s where medical support becomes absolutely crucial.
You see, OWCP claims live or die on medical documentation. Not your description of the pain (though that matters), not your supervisor’s incident report (though that helps), but on what medical professionals can document, measure, and explain. Think of it like this: you might know your ankle hurts every time it rains, but the claims examiner needs to see X-rays showing arthritis, MRI results revealing damaged cartilage, or a doctor’s report connecting your current symptoms to that fall you took in the warehouse.
But here’s what gets tricky – and this is where a lot of people get blindsided. Sometimes you don’t realize you need additional medical support until you’re already deep in the claims process. Maybe your initial treatment seemed to work, so you thought you were good to go. Or perhaps your symptoms evolved over time, developing into something more complex than anyone anticipated. Suddenly, you’re dealing with denied treatments, questioned diagnoses, or requests for independent medical examinations that feel more like interrogations.
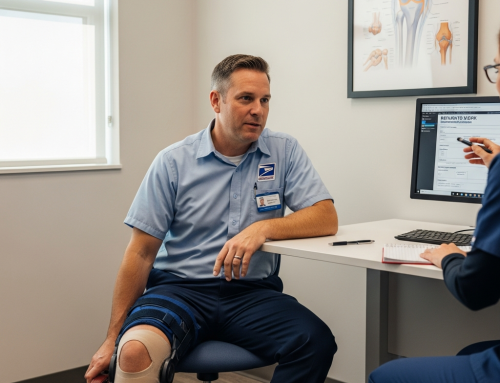
I remember talking to a postal worker who thought his repetitive stress injury was straightforward – just some wrist pain from sorting mail. Six months later, he was dealing with nerve damage that affected his entire arm, sleep disruption from chronic pain, and a claims examiner who kept questioning why he needed ongoing treatment for “just a sore wrist.” That’s when he realized his case had moved way beyond simple documentation into territory that required serious medical advocacy.
The truth is, there are specific warning signs that your OWCP claim needs stronger medical support. Maybe you’re already seeing them in your own situation – those moments when you think, “Something’s not right here,” or “This is taking way longer than it should.” These red flags don’t necessarily mean your claim is doomed, but they do mean it’s time to get proactive about building a stronger medical foundation for your case.
In the next few minutes, we’re going to walk through seven key signs that indicate your claim needs additional medical support – from the obvious ones (like outright denials) to the more subtle signals that experienced claims advocates recognize but that might slip past someone handling their first workplace injury. More importantly, we’ll talk about what you can actually *do* about each situation.
Because here’s what I believe: you shouldn’t have to become a legal expert or a medical researcher just because you got hurt at work. But you do need to know when your case requires more firepower than basic documentation…
The Maze of Federal Worker Compensation
Look, OWCP claims aren’t exactly… straightforward. If you’re a federal employee who’s been injured on the job, you’ve probably discovered that the Office of Workers’ Compensation Programs operates in its own universe – one where logic sometimes takes a backseat to bureaucracy.
Think of OWCP like that friend who’s super generous but also incredibly particular about how you ask for help. They’ll absolutely cover your medical expenses and lost wages, but only if you follow their very specific rules. Miss a step? Good luck explaining yourself later.
The thing is, most people assume that getting hurt at work automatically means you’re covered. And technically, you’re right – but there’s a canyon-sized gap between being eligible for benefits and actually receiving them. That’s where the real challenge begins.
What Makes Medical Evidence So Critical
Here’s something that catches nearly everyone off guard: OWCP doesn’t just want proof that you’re injured. They want proof that your injury is work-related, that it’s as severe as you claim, and that your treatment plan makes sense.
It’s like being asked to prove not just that your car is damaged, but that the specific pothole caused the damage, that the damage affects your ability to drive, and that the repair shop you chose knows what they’re doing. Exhausting? Absolutely.
The medical evidence becomes your translator in this bureaucratic conversation. Without it, you’re essentially telling OWCP, “Trust me, I’m hurt” – and unfortunately, they don’t operate on the trust system.
The Documentation Dance
Every OWCP claim lives or dies by its paperwork. I know, I know – you’re dealing with pain, missing work, worried about bills, and the last thing you want to think about is filing systems. But here’s the reality: OWCP processes thousands of claims, and they need a paper trail that clearly tells your story.
Medical records serve as the backbone of this documentation. They’re not just random doctor’s notes – they’re legal documents that establish timelines, connect symptoms to workplace incidents, and justify treatment decisions. Think of them as the breadcrumbs that lead OWCP through the forest of your case.
But here’s where it gets tricky… not all medical documentation is created equal in OWCP’s eyes. A quick urgent care visit might document that you’re in pain, but it doesn’t necessarily establish the work-relatedness they’re looking for. This is why understanding what kind of medical support you need becomes crucial.
When Your Case Gets Complicated
Some injuries are pretty straightforward – you slip on a wet floor, break your wrist, get an X-ray showing the break. Case closed, right? Well, usually. But what about when you develop chronic pain months later? Or when that “minor” back strain turns into something requiring surgery?
This is where many OWCP claims hit turbulence. Delayed symptoms, pre-existing conditions, or injuries that worsen over time can make even the most legitimate claim look questionable without proper medical backing.
Actually, that reminds me of something important – OWCP operates under the assumption that people might exaggerate their injuries. I’m not saying it’s fair, but it’s reality. They’ve built their system around requiring proof for everything, which means your medical team needs to be incredibly thorough in their documentation.
The Ripple Effect of Inadequate Support
When your medical evidence is weak or incomplete, it doesn’t just slow down your claim – it can create a domino effect that impacts every aspect of your case. Benefit payments get delayed, treatment approvals take forever, and you might find yourself fighting battles you never saw coming.
I’ve seen people go months without proper treatment because their initial medical report didn’t clearly establish work-relatedness. Others have had their benefits suddenly stopped when OWCP decided their ongoing treatment wasn’t medically necessary – even though they were still in significant pain.
The frustrating part? Many of these issues could have been prevented with the right medical support from the beginning. It’s like building a house – you can’t just slap a beautiful facade on a shaky foundation and expect it to stand up to scrutiny.
Your OWCP claim isn’t just about getting immediate medical care covered. It’s about protecting your long-term financial stability and ensuring you have access to the treatment you need for as long as you need it. That’s why recognizing when your claim needs stronger medical support isn’t just helpful – it’s essential.
Getting Your Doctor on Board (Before They Even Know They Need to Be)
Here’s something most people don’t realize – your doctor probably has zero experience with OWCP claims. I mean, why would they? They went to medical school to heal people, not navigate federal bureaucracy. So you need to become their unofficial OWCP translator.
Start by bringing documentation to every appointment. Not just your claim number (though definitely bring that), but a simple timeline of your injury and how it affects your daily work tasks. Write it down beforehand because – trust me – you’ll forget half of it once you’re sitting in that examination room wearing a paper gown.
The magic phrase you want to use with your doctor is this: “Can you document in my chart how this injury specifically prevents me from performing my essential job functions?” Don’t just say you’re in pain. Pain is subjective. But if you can’t lift 50 pounds because of your back injury, and your job requires lifting mail sacks… well, that’s concrete evidence OWCP can’t argue with.
The Art of Medical Record Requests (It Really Is an Art)
Most people think requesting medical records is straightforward. Ha. It’s more like trying to solve a puzzle where half the pieces are hidden and the other half are in different languages.
First, always request your records in writing – even if they say you can just call. Verbal requests disappear into the ether. Written requests create a paper trail, and paper trails win claims.
When you request records, be specific about dates, but cast a wide net. Don’t just ask for records from the day you got hurt. Ask for records from three months before your injury through the present. Why? Because sometimes your doctor mentioned symptoms or concerns that foreshadowed your workplace injury, and that context can be golden.
Here’s a insider tip: many medical offices will give you copies for free if you frame it as “continuing care” rather than “legal purposes.” Just saying…
Building Your Medical Timeline Like a Detective
Think of yourself as building a case file – because essentially, that’s what you’re doing. Create a simple spreadsheet (or even just a notebook) with three columns: Date, Medical Event, and Impact on Work.
Every doctor visit, every symptom flare-up, every day you couldn’t perform your regular duties… it all goes in there. Include seemingly minor things too. That physical therapy session where you couldn’t complete the exercises? Document it. The day you had to ask a coworker to lift something for you? Write it down.
The goal isn’t to create a medical textbook – it’s to show a clear pattern of how your injury consistently affects your ability to work. OWCP loves patterns because patterns are hard to fake or exaggerate.
Second Opinions: When and How to Get Them
Sometimes your treating doctor is… well, let’s just say they’re not giving you the support you need. Maybe they’re dismissive, maybe they don’t understand workplace injuries, or maybe they’re just not documenting things the way OWCP needs to see them.
Getting a second opinion isn’t admitting defeat – it’s being smart. But here’s the thing: you can’t just doctor-shop until someone tells you what you want to hear. That looks suspicious and actually hurts your case.
Instead, approach it strategically. If your primary doctor is a family practitioner and you have a complex orthopedic injury, requesting a specialist consultation is completely reasonable. If you’ve been treating conservatively for months without improvement, asking for a different perspective makes sense.
The Follow-Up Game (Because One Visit Is Never Enough)
Here’s what I see people do wrong all the time: they go to the doctor once, get a diagnosis, and think they’re done. Nope. OWCP wants to see consistent medical care and ongoing documentation of your condition.
This doesn’t mean you need to become a hypochondriac, but it does mean you need to be proactive about follow-ups. If your doctor says “come back in six weeks,” actually go back in six weeks. If symptoms worsen or new issues develop, get them documented immediately.
Think of it this way – if you told your boss you needed time off for a medical condition but then never saw a doctor again, wouldn’t that seem suspicious? OWCP thinks the same way.
The key is creating a medical record that tells a consistent, believable story about someone who’s genuinely injured and actively seeking appropriate treatment. Because at the end of the day, that’s exactly what you are.
When Documentation Feels Like a Foreign Language
Let’s be honest – the paperwork alone can make you want to crawl back into bed and pretend your injury never happened. You’re dealing with pain, maybe missing work, and suddenly you’re expected to become fluent in medical terminology and federal claim procedures? It’s like being asked to perform surgery while riding a unicycle.
The biggest stumbling block I see? People think they need to figure it all out themselves. You don’t. Your doctor’s office has staff who’ve dealt with workers’ comp claims before – lean on them. Ask your physician’s assistant or nurse to explain what they’re documenting and why. Most healthcare providers want to help; they just need to know you’re struggling with the process.
Here’s what actually works: bring a notebook to appointments. Not for looking studious (though that’s nice), but because when you’re in pain, your brain isn’t filing information properly. Write down what the doctor says about your restrictions, treatment plans, even their casual observations. Those offhand comments about your range of motion? Pure gold for your claim.
The “It’s Not That Bad” Trap
This one breaks my heart every time. You downplay your symptoms because you don’t want to seem dramatic, or maybe you’re genuinely unsure if what you’re experiencing is “worth” mentioning. Meanwhile, your claim examiner is reading between the lines of your medical records, looking for evidence that matches your reported limitations.
I’ve watched perfectly valid claims get delayed because someone said “I’m fine” when asked about pain levels, thinking they were being brave. But here’s the thing – you’re not applying for a stoicism award. You’re documenting an injury that’s affecting your ability to work and live normally.
The solution isn’t to exaggerate (please don’t), but to be brutally honest about your bad days, not just your good ones. Keep a simple pain diary on your phone. Rate your pain level each morning and evening. Note what activities make it worse. When you tell your doctor that lifting anything over ten pounds sends shooting pain down your arm… that’s not complaining, that’s providing crucial medical information.
When Your Doctor Seems to Be Phoning It In
Sometimes you’ll get a healthcare provider who treats workers’ comp cases like they’re checking boxes rather than treating a human being. Short appointments, minimal documentation, vague treatment plans – it happens more than it should.
You have options, and the first one might surprise you: speak up during the appointment. Say something like, “I’m concerned my work restrictions aren’t clearly documented. Could you help me understand what activities I should avoid?” Most doctors will snap to attention when they realize you’re paying attention to the details that matter for your claim.
If that doesn’t work… well, you’re not married to your first choice of physician. OWCP allows you to change doctors, though there’s a process. Sometimes getting a second opinion – even if you stick with your original doctor – can provide the detailed documentation your claim needs.
The Waiting Game That Tests Your Sanity
Let’s talk about something nobody warns you about: the psychological toll of waiting. You file your claim, submit your medical evidence, and then… silence. Weeks pass. Maybe months. Meanwhile, bills are piling up, and you’re starting to wonder if you imagined the whole thing.
This is where having realistic expectations saves your mental health. Initial claim decisions can take 30-45 days, sometimes longer if they need additional medical information. Appeals? Add several more months to that timeline.
But here’s what you can control: stay organized and proactive. Follow up every two weeks (not every day – that’s how you become “that person” in the claims office). Keep copies of everything you submit. When you call for updates, have your claim number ready and ask specific questions: “Has my medical report from Dr. Smith been received? Do you need any additional documentation from me?”
When Everyone Becomes an Expert
Suddenly, your coworker’s cousin who “went through the same thing” is giving you legal advice. Your neighbor knows someone who “beat the system.” Uncle Bob has opinions about what you should and shouldn’t say to doctors.
Here’s the truth: every workers’ comp case is different. Your specific injury, your job duties, your medical history – it all matters. Well-meaning advice from people who aren’t medical professionals or claims specialists can actually hurt your case.
Instead, build your team: your treating physician, maybe a workers’ comp attorney if things get complicated, and the claims representative who’s actually handling your case. These are the voices that matter. Everyone else? Thank them for caring and change the subject.
What Happens After You Connect with Medical Support
So you’ve recognized the signs and decided it’s time to get proper medical backing for your OWCP claim. Good for you – but let’s be real about what comes next. This isn’t going to be an overnight transformation, and anyone who tells you otherwise is selling something.
First things first: finding the right medical provider who understands federal workers’ comp can take some time. You’re not just looking for any doctor – you need someone who speaks OWCP’s language and won’t get frustrated when the paperwork starts piling up. Most quality providers who work with federal employees are pretty busy (because, well, they’re good at what they do), so you might be looking at 2-4 weeks for an initial appointment.
The Documentation Process Takes Time – And That’s Normal
Once you’re connected with the right medical team, expect the documentation process to unfold over several weeks or even months. Your doctor needs to understand your case thoroughly before they can write compelling reports. This means multiple appointments, possibly some additional testing, and a lot of detailed conversations about how your injury affects your daily work and life.
I know it’s tempting to rush this part – especially when you’re dealing with claim denials or delayed benefits. But here’s the thing: a rushed medical report that misses key details can actually hurt your case more than help it. Your doctor needs time to paint a complete picture of your condition and its connection to your work duties.
You’ll probably find yourself repeating your story several times to different people in the medical office. The intake coordinator, the physician’s assistant, the doctor… it can feel repetitive, but each person is gathering different pieces of information that’ll eventually come together in your medical documentation.
Working with Your Medical Team
Here’s what I wish more people knew going into this: your relationship with your medical provider is a partnership. They bring the clinical expertise, but you bring the detailed knowledge of how your injury impacts your specific job duties.
Come prepared to your appointments with specifics. Not just “my back hurts” but “I can’t lift the 30-pound case files from the bottom shelf anymore, and when I try to sit at my computer for more than an hour, the pain shoots down my left leg.” The more concrete examples you can provide, the better your doctor can connect your symptoms to functional limitations.
Don’t be surprised if your doctor asks questions that seem unrelated to your injury at first. They might want to know about your sleep patterns, your mood, how you’re managing at home… This isn’t them being nosy. Chronic pain and work injuries affect your whole life, and documenting these impacts strengthens your case.
Timeline Realities You Should Know
Most people see some movement in their case within 60-90 days of getting proper medical support, but “movement” doesn’t necessarily mean “resolution.” You might see OWCP requesting additional information, scheduling an independent medical exam, or asking for clarification on certain points. This is actually progress – it means they’re actively reviewing your case rather than letting it sit in a pile.
If your case has been denied before, the appeals process can take several months even with strong medical documentation. I know that’s not what you want to hear, but it’s better to have realistic expectations than to set yourself up for disappointment.
Staying Organized Through the Process
You’re going to accumulate a lot of paperwork – medical reports, correspondence with OWCP, updated claim forms. Start a simple filing system now, because trying to find that one important document when OWCP calls? Not fun.
Keep copies of everything you send to OWCP, and don’t be afraid to follow up if you haven’t heard back in a reasonable timeframe. Squeaky wheel and all that…
When Things Don’t Go According to Plan
Sometimes even with excellent medical support, cases hit unexpected snags. Maybe OWCP wants additional testing. Maybe they disagree with your doctor’s assessment. This doesn’t mean you’ve failed or that your medical team isn’t doing their job – it’s just part of navigating a complex system.
The key is maintaining open communication with your medical provider throughout the process. They’ve likely seen whatever curveball OWCP throws, and they’ll know how to adjust their approach accordingly.
Remember, getting proper medical support significantly improves your chances of a successful outcome, but it doesn’t guarantee a specific timeline. Focus on building the strongest case possible rather than rushing toward an arbitrary deadline.
You know what? Dealing with an OWCP claim while you’re already managing pain, uncertainty, and maybe even financial stress… it’s honestly overwhelming. And here’s the thing – you shouldn’t have to figure this out alone.
Those seven signs we talked about? They’re not meant to scare you. Think of them more like warning lights on your car dashboard. When that check engine light comes on, you don’t panic and assume your car is totaled. You take it to someone who knows what they’re looking at. Same principle applies here.
The reality is that federal workers’ compensation cases can be incredibly complex – and that’s putting it mildly. There are forms that seem designed to confuse, deadlines that creep up faster than you’d expect, and medical requirements that… well, let’s just say they weren’t written with regular people in mind. It’s like trying to navigate a maze while blindfolded.
But here’s what I’ve learned from years of helping people through this process: you have more power than you think. Even when OWCP denies your claim or questions your injury, even when you’re drowning in paperwork, even when it feels like the whole system is working against you – there are ways to turn things around.
The medical support piece? That’s often the game-changer. Because when you have the right documentation, the right medical professionals who understand both your condition AND the federal workers’ comp system… suddenly those seven warning signs start looking less like roadblocks and more like stepping stones.
I think about Sarah (not her real name, but her story is real) – a postal worker who came to us after two claim denials. She’d been dealing with chronic back pain for months, trying to push through because she needed the income. Her family doctor was great, but he didn’t quite understand what OWCP needed to see in his reports. Fast forward six months with proper medical support, and not only was her claim approved, but she also got the treatment that actually helped her pain.
That’s the thing about getting the right help – it’s not just about winning your case (though that matters, obviously). It’s about getting your life back. Getting the treatment you need. Having someone in your corner who speaks the language of federal bureaucracy so you don’t have to learn it the hard way.
Look, I get it if you’re hesitant about reaching out for help. Maybe you’re worried about costs, or you think you should be able to handle this yourself, or you’re just tired of explaining your situation to yet another person who might not get it.
But what if – and I know this might sound too good to be true – what if getting help actually made things easier instead of more complicated? What if you could hand over the paperwork headaches to someone who’s dealt with hundreds of cases just like yours?
If any of those seven signs rang true for you, or if you’re just feeling stuck and frustrated with where your claim stands right now… maybe it’s time to have a conversation with someone who can help. Not because you’re failing at handling this yourself, but because you deserve support.
We’re here when you’re ready. No pressure, no judgment – just real help for real people dealing with really challenging situations.